
At the office of Vaccaro Aesthetic and Family Dentistry, our first priority is preserving natural teeth whenever doing so serves a patient’s long-term health and function. Still, there are times when removal is the safest, most predictable option. We approach every extraction with careful evaluation, clear explanation, and a focus on minimizing discomfort and preserving the surrounding tissues.
Deciding to remove a tooth is never taken lightly. Before recommending extraction, we complete a thorough review of your medical and dental history, perform an in‑office examination, and use imaging to see the tooth and its supporting structures in detail. That broad perspective helps us choose the least invasive, most effective plan for your particular situation.
When extraction is recommended, our goal is to make the process as straightforward and comfortable as possible—whether that means a simple in‑office removal or a coordinated referral for a surgical extraction. We discuss alternatives, anticipated outcomes, and the best options for replacing the tooth when appropriate, so you can make a confident, informed decision about your care.
Primary teeth that fail to fall out or are severely decayed
Sometimes a primary ("baby") tooth does not loosen as expected because its roots didn’t resorb or because it has become fused to the jawbone. When an over‑retained primary tooth blocks the eruption path of the permanent tooth or causes alignment issues, careful extraction can allow normal development to continue and prevent future orthodontic problems.
Permanent teeth with extensive, non-restorable damage
When decay, trauma, or structural breakdown leaves too little healthy tooth to support a reliable restoration, removal may be the best option. Extracting a non‑restorable tooth prevents ongoing infection and pain, and it allows us to plan predictable replacement options that restore function and appearance.
Teeth fractured below the gum line or with irreparable root damage
Cracks and fractures can vary widely in severity. If a fracture involves the root or extends beneath the gum so that restoration won’t provide lasting strength, extraction is often the most practical and durable choice. Removing a compromised tooth can protect nearby teeth and reduce the risk of recurrent infections.
Advanced periodontal disease undermining tooth support
When periodontal disease has significantly diminished the bone and soft tissue that hold a tooth in place, extraction may be necessary to stop the spread of infection and to preserve overall oral health. In many cases, removing a loose, diseased tooth improves comfort and makes restorative or reconstructive work more predictable.
Impacted or problematic wisdom teeth
Third molars often erupt without enough room, sit at awkward angles, or are partially covered by gum tissue—conditions that can lead to decay, infection, pain, or damage to adjacent teeth. Addressing troublesome wisdom teeth early, especially in younger adults, often prevents more complex problems down the road.
Extractions as part of orthodontic planning
In some cases a crowded bite results from a mismatch between tooth size and jaw size. To achieve the best long‑term alignment and bite function, removing one or more teeth can be an intentional, carefully planned step in an orthodontic treatment strategy.
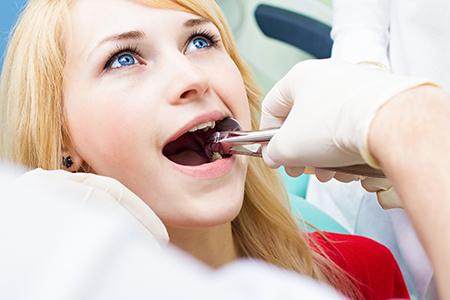
Good outcomes begin with a careful assessment. That means reviewing your medical history, medications, and any conditions—such as heart, bleeding, or immune disorders—that may affect treatment. We also ask about recent illnesses and coordinate with your physician when medical clearance or special precautions are needed.
Imaging plays a central role in planning. Digital radiographs let us view root shape, root position, and the relationship of a tooth to nearby anatomic structures. This information helps us determine whether an extraction will be straightforward or if a surgical approach is likely to be required.
We review anesthetic options and comfort measures before any procedure. Local anesthesia is standard and effective for most extractions; for anxious patients or more complex cases, we discuss additional sedation choices to ensure a calm, controlled experience. Expect a clear explanation about what to expect before, during, and after the appointment so you feel prepared and supported.
When a tooth presents unusual anatomy, is deeply broken, or is impacted, we’ll explain if a referral to an oral surgeon is the most appropriate path. That collaboration ensures each patient receives care from the clinician best suited to the technical demands of the case.
Simple extractions are performed when the tooth is fully visible and the roots are accessible. After numbing the area with a local anesthetic, your dentist gently loosens the tooth and removes it using specialized forceps. The process is efficient, and most patients experience only brief pressure and minimal discomfort.
Surgical extractions are indicated for teeth that are impacted, broken at the gum line, or fused to the jaw. These procedures may require a small incision, removal of a bit of bone, or sectioning the tooth into parts for safe removal. Local anesthesia is always used, and sedation can be arranged when needed. For complex cases we may refer you to a qualified oral and maxillofacial surgeon who specializes in these procedures.
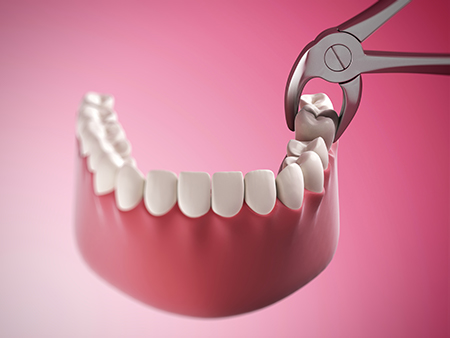
Healing after an extraction follows a predictable pattern, and most patients recover quickly when they follow basic aftercare. We provide clear, written post‑operative instructions tailored to your procedure. These guidelines aim to minimize bleeding and swelling, manage discomfort, protect the developing clot at the extraction site, and reduce the risk of infection.
In the hours after surgery, resting with your head elevated and applying controlled ice to the face can limit swelling. It’s important to avoid actions that disturb the clot—such as rinsing vigorously, using a straw, or smoking—because the clot is a critical early step in tissue repair.
Pain is typically well controlled with over‑the‑counter medications, unless a prescription is necessary for a more involved procedure. If antibiotics are prescribed, take the full course exactly as directed. Keep in close contact with us if your pain, swelling, or bleeding is unusual or if you develop new symptoms.
We schedule follow‑up visits when appropriate to check healing and remove sutures if they were placed. During your visit we’ll also discuss long‑term planning—whether that means monitoring the site, restoring the area with an implant, bridge, or denture, or planning orthodontic steps to optimize function and esthetics.
Control bleeding with gauze
Bite gently on a gauze pad placed over the extraction site for the time recommended by your clinician. If bleeding persists, replacing the gauze and applying steady pressure usually helps. Contact our office if bleeding remains heavy after following instructions.
Protect numb tissues
Avoid chewing or touching the area while local anesthesia lasts to prevent accidental biting of lips, tongue, or cheeks.
Follow medication directions
Take any prescribed antibiotics or pain medications exactly as directed. If asked to use an over‑the‑counter analgesic before the anesthetic wears off, this can reduce peak discomfort.
Protect the blood clot
Avoid spitting, rinsing forcefully, drinking through a straw, or sucking on candies for at least 24 hours so the clot can stabilize.
Limit swelling with ice
Apply an ice pack to the cheek in short intervals during the first 24 hours to reduce facial swelling.
Don't smoke
Smoking impairs blood clot formation and delays healing. Avoid tobacco use for at least one week after surgery, or longer if advised.
Eat soft, soothing foods
Start with cool or lukewarm, soft foods and avoid hot, spicy, or crunchy items until the site has had time to begin healing.
Maintain gentle oral hygiene
Keep the mouth clean with gentle brushing away from the extraction area; when advised, use a mild saline rinse to help keep the area fresh without disturbing the clot.
Attend follow-up care
Return for any scheduled post‑operative check so we can monitor healing, remove sutures if needed, and plan next steps for replacement or further treatment.
If you notice increasing pain, prolonged heavy bleeding, fever, or any changes that concern you, contact the office promptly so we can evaluate and advise next steps.
When a tooth must be removed, you deserve care that balances clinical rigor with compassion and clear communication. Our team focuses on gentle technique, thoughtful treatment planning, and honest discussion about replacement options when needed. We’ll explain choices such as removable dentures, fixed bridges, and dental implants so you understand the benefits and what to expect from each approach.
Whether your care remains in our office or we coordinate with a specialist for complex surgical needs, we manage each step to protect your comfort and long‑term oral health. Our aim is to restore function and appearance in a way that supports your lifestyle and confidence.
To learn more about extractions or the restorative options that follow, please contact us for additional information. Our team is available to answer questions and help you make the right choice for your smile.

Removing a tooth becomes the healthiest option when preservation would compromise long-term oral health or lead to ongoing infection or pain. Common reasons include teeth that are extensively decayed and non-restorable, fractures that extend below the gum line, advanced periodontal disease, or primary teeth that obstruct normal development. The decision follows a careful evaluation of the tooth, surrounding tissues, and overall treatment goals to choose the least invasive yet most reliable solution.
Before recommending extraction, we review your full medical and dental history, perform a clinical exam, and obtain imaging to understand root structure and nearby anatomy. We discuss alternatives, anticipated outcomes, and the implications for chewing, alignment, and future restorative work so you can make an informed choice. When removal is the best path, planning focuses on minimizing trauma and preserving the supporting tissues for optimal healing and future treatment options.
Evaluation begins with a detailed review of medical history, medications, and any conditions that could affect treatment, such as heart, bleeding or immune disorders. Digital radiographs or 3D imaging are used to assess root shape, proximity to nerves or sinuses, and whether the tooth is impacted or broken; this information guides the clinical approach. We also discuss anesthesia and comfort options, coordinate with medical providers when needed, and explain what to expect before, during, and after the procedure.
Planning emphasizes minimizing risk and selecting the clinician best suited to the case, whether the extraction can be completed in our office or if a referral is more appropriate. The chosen plan includes steps to protect adjacent teeth and tissues and to preserve options for future restoration, such as implants or bridges. Clear communication and shared decision-making are central to achieving predictable, safe outcomes.
A simple extraction is performed on a tooth that is fully erupted and easily accessible; after local anesthesia, the dentist uses elevators and forceps to loosen and remove the tooth with minimal tissue manipulation. Patients typically experience brief pressure rather than sharp pain, and the procedure is efficient with straightforward healing. Simple extractions are common for teeth that have sufficient clinical crown and normal root anatomy.
Surgical extractions are required when a tooth is impacted, fractured at or below the gum line, or has complex root anatomy; these procedures may involve a small incision, removal of a bit of bone, or sectioning the tooth into parts for safe removal. Local anesthesia is always used, and sedation or referral to an oral surgeon can be arranged for more complex cases or anxious patients. Surgical extractions generally have a slightly longer healing period and may require sutures and additional aftercare instructions.
Local anesthesia is the standard for most extractions and provides reliable numbness of the tooth and surrounding tissues so the procedure is comfortable. For patients with dental anxiety or for more involved surgical cases, additional options such as oral sedation or nitrous oxide may be offered to promote relaxation and reduce stress. Intravenous sedation or general anesthesia can be arranged when clinically appropriate, typically in coordination with a qualified sedation team or specialist.
We review the risks and benefits of each option and tailor the approach to the patient’s medical history, level of anxiety, and the complexity of the extraction. Instructions about fasting, accompanying adults, and medication adjustments are provided when sedation is planned to ensure safety. Our goal is to maintain a calm, controlled experience while prioritizing patient comfort and clinical effectiveness.
If you take anticoagulant or antiplatelet medications, have a bleeding disorder, or manage cardiac or immune conditions, disclose these details during your consultation so we can coordinate care. Some situations require communication with your prescribing physician to determine whether medication adjustments or special precautions are needed before the procedure. We balance the risk of bleeding with the risk of altering medications and follow current medical guidelines to reduce complications.
During evaluation we may request laboratory tests, schedule additional monitoring, or plan for hemostatic measures during and after the extraction to control bleeding. Clear preoperative instructions are provided to reduce risk, and we arrange appropriate follow-up to check healing. If medical clearance or specialized management is necessary, we will obtain it before proceeding to ensure patient safety.
Initial recovery typically involves a predictable sequence of clot formation, tissue repair, and gradual reduction of swelling and discomfort over several days. For most patients, over-the-counter analgesics and cold packs control pain and swelling effectively; stronger prescription medications are reserved for more involved procedures when needed. Rest, head elevation, and limited physical exertion during the first 24–48 hours support healing and comfort.
We provide specific written aftercare instructions to protect the clot, manage medications, and reduce the risk of complications such as infection or dry socket. Avoiding actions that disturb the clot—like vigorous rinsing, using a straw, or smoking—is important during early healing. If pain, swelling, or bleeding is unusually heavy or prolonged, contact us promptly so we can assess and intervene if necessary.
Preventing dry socket and infection centers on protecting the blood clot and practicing careful oral hygiene that avoids disturbing the extraction site during the early healing phase. Follow instructions to avoid spitting, using straws, or smoking for at least 24–72 hours and to perform gentle rinses only when recommended by your clinician. Taking any prescribed antibiotics exactly as directed and using recommended antiseptic rinses can further reduce infection risk when clinically indicated.
Applying ice during the first 24 hours, adhering to a soft-food diet, and attending scheduled follow-up visits help monitor healing and catch problems early. If you notice increasing pain that radiates to the ear, visible bone, persistent bad taste, or delayed healing, contact the office so we can evaluate for dry socket or infection and provide appropriate care. Prompt assessment and treatment usually restore healing and reduce discomfort quickly.
Replacing an extracted tooth depends on its location, your bite, esthetic concerns, and long-term function; some spaces may be monitored while others benefit from prompt restoration to prevent shifting and preserve chewing efficiency. Common replacement options include dental implants, fixed bridges, and removable dentures, each with distinct clinical requirements and benefits. The timing of replacement is planned based on healing, bone volume, and any additional procedures such as grafting that may be recommended.
We discuss the pros and cons of each restorative approach and plan the sequence of care to optimize outcomes, including preserving bone and soft tissue for an implant when appropriate. Collaboration with specialists occurs when needed to coordinate implant placement or complex restorative steps. Your clinician will outline realistic expectations for function, appearance, and maintenance so you can choose the option that best fits your needs and lifestyle.
Yes, referrals are sometimes the most appropriate option when an extraction involves unusual anatomy, deeply impacted teeth, proximity to nerves or sinuses, or other technical complexities that require advanced surgical expertise. In such cases we coordinate care with experienced oral and maxillofacial surgeons to ensure safe, predictable results and to address any sedation or anesthesia needs beyond in‑office capabilities. Referrals allow patients to receive treatment from the clinician best suited to the technical demands of the case while maintaining continuity of care.
For routine or less complex extractions, the procedure can often be completed safely in our office with local anesthesia and available sedation options. Whether care stays in our office or involves a specialist, we manage planning, communication, and follow-up to protect your comfort and long‑term oral health. When a referral is recommended, we explain the reasons and help arrange appointments and information transfer for a smooth experience.
Pediatric extractions take into account the child’s dental development, behavior, and the status of developing permanent teeth; primary teeth that fail to shed or that block eruption may be removed to allow normal growth. Behavior management techniques, child‑appropriate communication, and sometimes nitrous oxide or mild sedation are used to reduce anxiety and ensure cooperation during the procedure. The clinician also evaluates whether space maintenance or coordination with orthodontic treatment will be necessary following extraction.
We provide parents with age‑appropriate aftercare instructions and monitor healing with follow-up visits to confirm normal development and eruption of permanent teeth. Decisions about timing and approach prioritize long‑term oral health and alignment while minimizing trauma and fear. When specialized care is required, we refer to pediatric dental or surgical specialists who have additional training in managing young patients.

Ready to book your next dental visit or learn more about our services?
Getting in touch with Vaccaro Aesthetic and Family Dentistry is quick and easy. Our friendly team is here to help with scheduling, answering questions about treatments, and addressing any concerns. Whether by phone or our convenient online form, we make connecting with us easy. Take the first step toward a healthier, more confident smile—contact us today and experience personalized dental care that truly makes a difference.