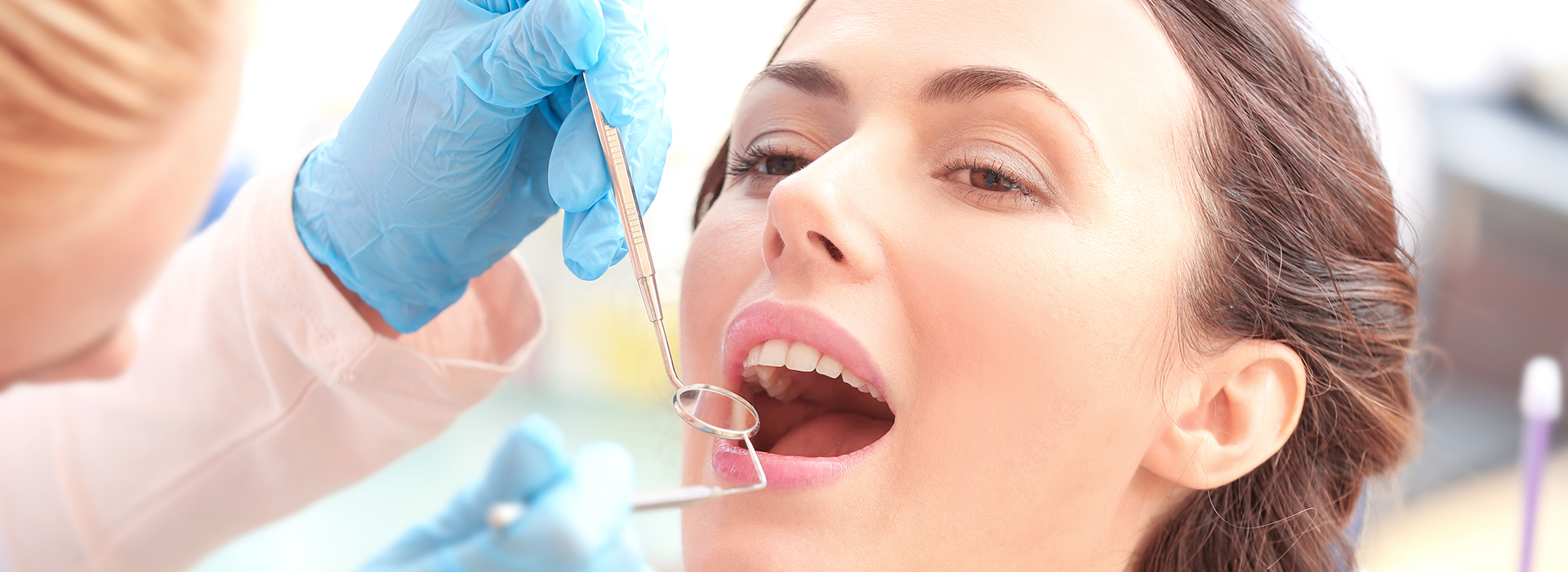
Gum disease is the leading cause of tooth loss in adults, yet it’s one of the most preventable oral conditions. Routine care, early detection, and targeted treatment can preserve your smile and protect your overall health. At Vaccaro Aesthetic and Family Dentistry, we emphasize practical, science-backed strategies to keep periodontal problems from taking hold and to restore health when they do.
Healthy gums form the foundation for a stable, functional, and attractive smile. When the tissues that surround and support the teeth remain healthy, chewing, speech, and daily comfort are preserved. Conversely, when inflammation takes hold, it undermines the structures that hold teeth in place and can lead to loosening and loss.
Gum disease is not isolated to the mouth. Research shows connections between chronic oral inflammation and broader health concerns, including cardiovascular disease, diabetes control, and respiratory conditions. Addressing periodontal issues is therefore an investment in both oral and overall well-being.
Prevention is straightforward and effective: consistent home care, regular professional cleanings, and early intervention when signs appear. With prompt attention, many cases can be managed without invasive procedures, and when more advanced care is needed, modern methods can restore function and appearance.
Periodontal disease often advances quietly; many people notice little or no pain until the condition becomes serious. Learning to recognize early warning signs gives you a chance to act before irreversible damage occurs. Regular checkups help catch subtle changes that might be missed at home.
Be especially attentive if you experience persistent gum bleeding, swelling, or a change in the way your teeth fit together. Bad breath that doesn’t improve with brushing, increased tooth sensitivity, or the development of gaps between teeth can also indicate progressing gum disease.
If you see any of these symptoms, schedule an evaluation—early treatment improves outcomes and reduces the need for complex interventions. Below are common indicators that warrant further assessment by a dental professional.
Inflamed, swollen, or unusually red gum tissue
Gums that bleed when brushing or flossing
Receding gum lines or roots becoming exposed
Increased sensitivity to hot, cold, or sweet foods
Persistent bad breath or an unpleasant taste in the mouth
Teeth that feel loose or shift position
New spacing between teeth or changes in your bite
Partial dentures that no longer fit comfortably
Pus or discharge near the gumline
Discomfort when biting or chewing

Gingivitis is the reversible, early stage of gum disease where inflammation is present but the supporting bone and connective tissues remain intact. Typical signs include redness, swelling, and bleeding that improve with better oral hygiene and professional care. Treating gingivitis promptly can prevent progression to more destructive stages.
If gingivitis is left unaddressed, it can progress to periodontitis, a condition in which pockets form between the teeth and gums and the underlying bone begins to resorb. As these pockets deepen, bacteria and toxins become more difficult to remove with routine brushing and standard cleanings, and damage accumulates.
Advanced periodontitis leads to pronounced gum recession, bone loss, and tooth mobility. At this stage, treatment objectives shift from simple reversal to stabilizing the disease, stopping further tissue breakdown, and restoring lost support where possible. Modern periodontal care aims to limit damage and rebuild structure using predictable techniques.
Because progression is often gradual and painless, regular periodontal screening during dental visits is essential. Measurements of pocket depth, radiographic imaging, and a careful periodontal chart together give a clear picture of disease activity and guide an appropriate, individualized plan of care.

When periodontal disease is identified early, conservative measures can be highly effective. Scaling and root planing—thorough cleaning below the gumline and smoothing of the tooth roots—removes the bacterial deposits that trigger inflammation and helps the tissues reattach to the tooth surface. These procedures are the cornerstone of non-surgical periodontal therapy.
Adjunctive therapies may include localized antimicrobial agents applied beneath the gums or short courses of systemic medication when appropriate. Improvements in home care, including targeted brushing and interdental cleaning, are a vital complement to in-office treatment and play a major role in preventing recurrence.
When non-surgical care achieves healthy pocket depths and stable tissue, patients transition to a maintenance program tailored to their needs. Periodic professional cleanings, monitoring of pocket depths, and reinforcement of home care maintain the gains achieved during active treatment.
Non-surgical treatment focuses on removing the biological triggers of disease and enabling healing. With proper instrumentation and technique, clinicians can reduce pocket depth and bacterial load without resorting to surgical intervention in many cases. This approach emphasizes effectiveness and minimal invasiveness.
Following active therapy, a structured maintenance schedule—often at more frequent intervals than standard cleanings—keeps plaque and calculus from reaccumulating below the gumline. Patients who adhere to this schedule typically experience better long-term stability and fewer complications over time.
Patient education is an integral component: learning precise flossing methods, choosing appropriate interdental aids, and understanding daily habits that influence periodontal health supports long-term success.
When pocket depths exceed what can be safely and effectively treated with non-surgical methods, surgical intervention may be recommended. Procedures such as flap surgery allow clinicians to access and thoroughly clean the root surfaces and reshape the supporting bone to reduce pocketing and improve hygiene access.
Regenerative techniques—bone grafts, guided tissue regeneration, and biologic agents—can encourage the body to rebuild lost bone and connective tissue when conditions are favorable. These procedures aim to restore stability and create a foundation for lasting oral health.
Contemporary surgical care is complemented by minimally invasive options and adjunctive technologies like dental lasers in selected cases. The choice of procedure is individualized based on the pattern of bone loss, aesthetic considerations, and the patient’s overall health.
Successful periodontal therapy depends on a partnership between clinician and patient. After active treatment, ongoing surveillance, consistent home care, and timely professional interventions prevent recurrence. Advances in imaging and diagnostics help clinicians detect subtle changes early and tailor maintenance intervals to individual needs.
In addition to traditional therapies, regenerative procedures and modern biomaterials offer meaningful options for rebuilding lost structure when indicated. Laser-assisted therapies and focused antimicrobial strategies can address challenging sites such as peri-implantitis and localized pockets while minimizing discomfort and recovery time.
Our team combines clinical experience with current technology to create treatment plans that reflect each patient’s goals and circumstances. When long-term stability is achieved, patients benefit from improved function, a more secure bite, and confidence in their oral health.
In summary, periodontal disease is common but manageable when detected early and treated with a consistent, evidence-based approach. If you have concerns about your gums or notice any of the signs described above, please contact us for more information about assessment and treatment options.

Periodontal disease is an infection of the gums and supporting structures around the teeth that begins with bacterial plaque buildup along the gumline. In its earliest stage, known as gingivitis, inflammation is confined to the soft tissues and is often reversible with proper cleaning and professional care. If left untreated, bacterial toxins and the body’s inflammatory response can destroy the connective tissues and bone that support teeth, leading to pocket formation and tooth mobility.
Development is usually gradual and influenced by factors such as poor oral hygiene, smoking, uncontrolled diabetes, certain medications, and genetic susceptibility. Regular dental visits that include periodontal screening allow clinicians to detect early changes and intervene before irreversible damage occurs. Early detection and treatment improve long-term outcomes and reduce the need for more invasive procedures.
Common signs that warrant a periodontal evaluation include gums that bleed with brushing or flossing, persistent redness or swelling, and gums that feel tender or pull away from the teeth. Patients may also notice bad breath that does not respond to routine hygiene, increased tooth sensitivity, gaps that develop between teeth, or changes in how partial dentures fit. Because periodontitis can progress painlessly, regular professional exams are important even when symptoms are mild or absent.
If you notice any of these warning signs, schedule an assessment so a clinician can measure pocket depths, review radiographs, and create an individualized plan. Early intervention typically limits tissue loss and simplifies treatment. Prompt attention also helps protect overall oral function and comfort.
Diagnosis begins with a thorough review of medical and dental history followed by a clinical periodontal exam that measures pocket depths, checks for bleeding on probing, assesses gum recession, and records tooth mobility. Dentists often supplement the exam with dental radiographs to evaluate bone levels and identify patterns of bone loss that are not visible clinically. Together these findings create a periodontal chart that quantifies disease activity and helps guide treatment decisions.
Additional diagnostic tools, such as specialized imaging, microbiological testing, or assessment of systemic risk factors like diabetes control, may be used in complex cases to refine the treatment approach. Accurate staging and grading of periodontal disease enable clinicians to recommend targeted therapies and appropriate maintenance intervals. Regular re-evaluation after treatment documents healing and helps prevent recurrence.
Non-surgical care focuses on removing the bacterial deposits that trigger inflammation and allowing the tissues to heal; the primary procedure is scaling and root planing, a deep cleaning below the gumline that smooths root surfaces to discourage bacterial reattachment. Clinicians may also use localized antimicrobial agents or prescribe short courses of systemic medication when indicated to reduce bacterial load and control infection. Patient education on effective home care, including proper brushing technique and improved interdental cleaning, is an essential complement to in-office therapy.
After active non-surgical therapy, patients typically enter a periodontal maintenance program with more frequent professional cleanings and monitoring than standard recall visits. This maintenance schedule helps prevent re-accumulation of plaque and identifies any sites that require further treatment. Many cases respond well to non-surgical measures when combined with consistent home care and regular follow-up.
Surgical treatment is considered when pocket depths and anatomical factors prevent adequate cleaning with non-surgical methods or when regenerative procedures are needed to restore lost support. Common surgical options include flap surgery to access and debride deep root surfaces, osseous contouring to reshape bone, and procedures to reduce pocket depth and improve long-term hygiene access. The specific approach is chosen based on the pattern of bone loss, aesthetic considerations, and the patient’s overall health.
Regenerative techniques such as bone grafting and guided tissue regeneration may be used during surgery to encourage the body to rebuild bone and connective tissue in favorable situations. Contemporary surgical care emphasizes minimally invasive methods and can incorporate adjunctive technologies like lasers in selected cases to reduce discomfort and support healing. A clear postoperative plan and maintenance schedule are essential components of successful surgical outcomes.
Regenerative procedures aim to restore the bone and soft tissue lost to periodontitis rather than simply halting disease progression, and they are most appropriate when defects have the shape and size that can support new tissue formation. Techniques include bone grafts, the use of barrier membranes for guided tissue regeneration, and biologic agents that stimulate healing and encourage new attachment. Success depends on careful case selection, stable wound management, and effective control of infection and inflammation.
Not every defect is amenable to regeneration; the clinician evaluates factors such as defect morphology, oral hygiene, smoking status, and systemic health when recommending these options. When successful, regenerative care can improve tooth stability and reduce the need for extraction or prosthetic replacement. Long-term monitoring and meticulous maintenance are required to preserve the gains achieved with regenerative therapy.
Chronic periodontal inflammation is associated with systemic effects and has been linked in research to conditions such as cardiovascular disease, poorer glycemic control in diabetes, and respiratory issues. The relationship is complex and appears to be bidirectional in some cases; for example, uncontrolled diabetes can worsen periodontal disease and periodontal inflammation can make blood sugar management more difficult. Addressing periodontal disease is therefore an important component of comprehensive health care and often involves communication with a patient’s medical providers when systemic risk factors are present.
Patients with chronic health conditions should inform their dental team so care can be coordinated and treatment plans adjusted safely. Periodontal therapy often improves oral inflammation and may contribute to better overall health markers when combined with appropriate medical management. Regular periodontal assessments are especially important for patients with systemic risk factors.
Yes. Dental implants can be affected by an inflammatory condition known as peri-implant mucositis or, if it progresses, peri-implantitis, which involves bone loss around the implant. Management begins with early detection and removal of plaque and calculus around the implant, improved home care, and the use of antiseptic or antimicrobial interventions. In more advanced peri-implantitis, surgical access, decontamination of the implant surface, and regenerative techniques may be necessary to control infection and restore lost structure when feasible.
Prevention relies on careful implant placement, regular professional maintenance, and patient adherence to meticulous oral hygiene practices. Patients with implants should remain in a tailored maintenance program to monitor soft tissue health and bone levels around the implant. Prompt attention to any signs of inflammation around an implant improves the likelihood of preserving the restoration.
Recovery varies with the type and extent of treatment but typically includes short-term sensitivity, mild swelling, and temporary changes in bite or chewing comfort that resolve as healing progresses. Clinicians provide postoperative instructions for pain control, oral hygiene adjustments, and dietary recommendations to support healing, and follow-up visits are scheduled to monitor tissue response. For surgical procedures, patients may receive specific wound-care guidelines and should expect periodic evaluations to assess regeneration and stability.
Long-term success depends on a structured maintenance plan that often includes more frequent professional cleanings and periodontal monitoring than standard recall intervals. Patients who commit to consistent home care, avoid tobacco, and manage systemic risk factors typically experience better stability and fewer complications. Ongoing communication with the dental team helps tailor maintenance intervals and detect any recurrence early.
Vaccaro Aesthetic and Family Dentistry emphasizes a collaborative approach to periodontal care by combining general dental expertise with specialized support when needed; the office hosts a periodontist once a week so patients can receive focused evaluation and treatment without an outside referral. This model streamlines care, facilitates timely intervention for complex cases, and allows the restorative and periodontal teams to plan coordinated treatment that addresses both function and aesthetics. Patients benefit from shared treatment planning and consistent follow-up within the same practice environment.
When advanced periodontal procedures are indicated, the team outlines the recommended options, explains expected outcomes, and establishes a clear timeline for active therapy and maintenance. The practice also customizes maintenance intervals and home care recommendations based on each patient’s disease risk and response to treatment. Clear communication, thorough documentation, and personalized follow-up are central to achieving durable periodontal health.

Ready to book your next dental visit or learn more about our services?
Getting in touch with Vaccaro Aesthetic and Family Dentistry is quick and easy. Our friendly team is here to help with scheduling, answering questions about treatments, and addressing any concerns. Whether by phone or our convenient online form, we make connecting with us easy. Take the first step toward a healthier, more confident smile—contact us today and experience personalized dental care that truly makes a difference.