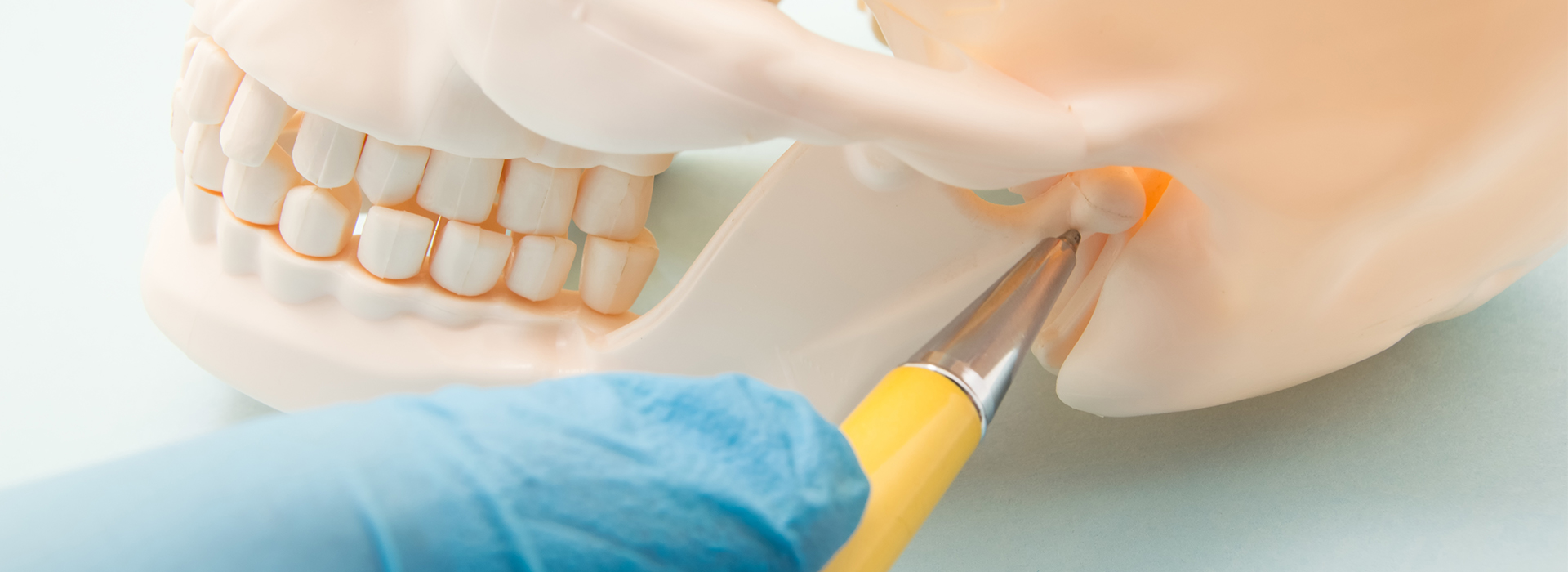
The temporomandibular joint (TMJ) is a compact but remarkably versatile structure that connects your lower jaw to the skull. Each person has two of these joints—one on either side of the face—and they operate together to allow chewing, speaking, yawning and the subtle movements needed for expression. Inside each joint sits a small, cushioned disc that helps absorb forces and guide smooth motion between the rounded condyle of the jaw and the temporal bone of the skull.
Because the TMJ must perform both hinge-like opening and closing motions as well as sliding movements from front to back and side to side, it is mechanically complex. That complexity means the joint depends on coordinated action among bones, cartilage, ligaments and the muscles of the face and neck. When any element in that system becomes strained or misaligned, the result can be pain, stiffness or a change in how the teeth come together.
Understanding the joint’s role in everyday function makes it easier to see why TMJ problems can affect more than just the jaw. Disruptions in this system can ripple outward, producing headaches, neck tension and even ear-related symptoms. A clear, practical view of jaw mechanics is the first step toward recognizing and addressing a disorder before it becomes chronic.
TMJ disorders rarely have a single cause; more often they arise from a combination of factors that place repeated stress on the jaw system. Chronic teeth grinding and clenching (bruxism) is a leading contributor, especially when it happens during sleep. Trauma to the jaw, such as a direct blow or a forceful opening of the mouth, can damage the joint or its disc and precipitate a long-lasting problem.
Systemic conditions also influence joint health. Certain forms of arthritis, including osteoarthritis and rheumatoid arthritis, can wear down joint surfaces or trigger inflammatory changes that affect TMJ function. Muscle tension related to stress, poor posture, or habitual behaviors like chewing gum can further aggravate the joint and surrounding tissues.
Individual anatomy and bite relationships matter, too. A misaligned bite or dental work that alters how teeth meet can change the distribution of forces across the jaw and TMJ. Age, genetics and prior dental history are all part of the overall risk profile. Because multiple elements can interact, a careful history and clinical exam are essential to identify the most likely contributors in each patient.
TMJ disorders can produce a broad spectrum of symptoms, which sometimes makes diagnosis challenging. Many people notice jaw-related signs first—aching pain around the joint, tenderness in the muscles used for chewing, or sensations of tightness. Clicking, popping or grating sounds when opening or closing the mouth are common, and for some people those noises accompany a feeling that the jaw “catches” or momentarily locks.
Because the TMJ sits close to the ears and the muscles of the head and neck, patients may report ear-related complaints such as a dull earache, fullness, or even ringing (tinnitus) without an active ear infection. Headaches and facial pain that concentrate around the temples or radiate into the neck and shoulders are also frequently tied to TMJ dysfunction. In more advanced cases, restricted opening or deviation in the jaw’s path may be obvious when a patient tries to yawn or bite.
The variability of symptoms is why a patient-centered approach matters: two people with similar joint changes on imaging may experience very different levels of pain or limitation. Early recognition of warning signs—particularly persistent pain, progressive difficulty opening, or symptoms that interfere with sleep or daily function—warrants professional evaluation to prevent worsening and to explore appropriate care options.
Not all jaw noises or mild discomfort indicate a progressive problem, but monitoring symptom patterns and noting triggers (chewing hard foods, long phone calls, stress) helps guide both diagnosis and self-management strategies.
A thoughtful, stepwise diagnostic process helps differentiate TMJ disorders from other causes of facial pain. Your dental provider will begin with a focused history to learn about symptom onset, duration, and factors that worsen or ease discomfort. This is followed by a hands-on clinical exam that assesses jaw range of motion, joint sounds, muscle tenderness and how the teeth come together during movement.
When indicated, targeted imaging provides additional detail. Standard radiographs may reveal joint alignment or bony changes, while advanced modalities such as cone beam computed tomography (CBCT) can offer precise views of bone structure. In some cases, magnetic resonance imaging (MRI) is used to visualize the soft tissue disc within the joint and to assess for internal derangement. Bite analysis and occlusal assessment may also be part of the workup to understand how dental relationships influence joint mechanics.
Because TMJ disorders often overlap with muscle-based pain and other conditions, collaboration with specialists—physical therapists, pain management clinicians, or ear/nose/throat providers—can be valuable. A comprehensive evaluation focuses not only on identifying structural issues but also on mapping functional contributors so treatment can be tailored to each patient’s needs.
Most people with TMJ problems respond well to conservative, reversible therapies aimed at reducing pain and restoring normal function. Oral appliances—such as night guards or stabilization splints—are commonly used to reduce excessive force on the joint and protect teeth from grinding. These devices are custom-made to fit the mouth and can relieve muscle tension and improve comfort, especially when combined with behavior change strategies.
Adjunctive treatments span a spectrum from physical therapy and guided stretches to targeted injections for persistent inflammation or muscle spasm. Simple self-care measures often provide meaningful relief: eating softer foods for a short period, avoiding wide yawns or hard-chewing foods, applying cold or moist heat as needed, and practicing relaxation or stress-reduction techniques to minimize clenching. Short-term use of over-the-counter anti-inflammatory medications may be recommended by a clinician when appropriate.
When conservative care does not sufficiently improve symptoms, more advanced options may be considered, including occlusal adjustment, orthodontic or prosthetic interventions to improve bite relationships, or referral for surgical consultation in rare, severe cases. Treatment plans should prioritize the least invasive, evidence-based approaches and be adapted over time in response to a patient’s progress.
At Vaccaro Aesthetic and Family Dentistry, we emphasize individualized care that integrates clinical evaluation, modern diagnostic tools and conservative therapies first. The goal is to restore comfortable function, reduce pain, and minimize the need for irreversible procedures whenever possible.
In summary, TMJ disorders encompass a range of conditions that affect jaw function and comfort. Because causes and symptoms vary widely, accurate assessment and a stepwise approach to care are essential. If you are experiencing persistent jaw pain, frequent headaches related to jaw movement, or changes in how your bite feels, please contact us to learn more about evaluation and the treatment options available.

The temporomandibular joint (TMJ) connects the lower jaw to the skull and enables actions such as chewing, speaking and yawning. Each person has two TMJs that work together to coordinate opening, closing and sliding movements. A small, cushioned disc inside the joint helps absorb forces and guide smooth motion between the condyle and the temporal bone.
Because the TMJ must perform hinge-like and gliding motions, it depends on coordinated action among bones, cartilage, ligaments and the muscles of the face and neck. When any part of this system becomes strained, misaligned or inflamed, movement can become painful or restricted. Understanding these mechanics helps patients recognize symptoms early and seek appropriate care before problems become chronic.
TMJ disorders usually arise from multiple contributing factors rather than a single cause. Chronic teeth grinding and clenching (bruxism), especially during sleep, is a common driver of joint and muscle strain. Direct trauma to the jaw or a forceful opening can injure the joint or its disc and trigger prolonged symptoms. Inflammatory conditions such as osteoarthritis or rheumatoid arthritis may also degrade joint surfaces and increase susceptibility to dysfunction.
Habitual behaviors like chewing gum, prolonged phone use that strains the jaw, and poor head or neck posture can aggravate TMJ symptoms over time. An individual's bite alignment and past dental work can change how forces are distributed across the TMJ and influence risk. Age, genetics and stress-related muscle tension further shape a patient’s overall risk profile.
Common symptoms include aching pain around the jaw, tenderness in the chewing muscles and sounds such as clicking, popping or grinding during jaw movement. Patients may notice limited opening, a jaw that feels stuck or deviation when opening widely, and increased discomfort when chewing. Because the TMJ is close to the ears and upper neck, complaints often include ear fullness, dull ear pain or ringing and headaches centered at the temples. Symptom intensity varies widely, which can make diagnosis based on symptoms alone challenging.
Watch for red flags such as steadily worsening pain, progressive loss of jaw opening, or symptoms that interfere with sleep or daily activities; these trends merit prompt evaluation. Not all jaw noises or mild soreness indicate a progressive disorder, but persistent or disabling signs should be assessed. Keeping a symptom diary that notes triggers and timing can help clinicians identify patterns during the diagnostic process.
A thorough evaluation begins with a detailed history about symptom onset, patterns and factors that worsen or relieve discomfort. The clinical exam assesses jaw range of motion, joint sounds and muscle tenderness while observing how the teeth come together during movement. Palpation of the temporomandibular joints and surrounding muscles helps pinpoint sources of pain and dysfunction. A dental provider will also look for signs of dental wear, recent orthodontic changes or other oral factors that could contribute.
Imaging is used selectively to add structural detail; panoramic radiographs and cone beam computed tomography (CBCT) can reveal bony changes or joint alignment issues. Magnetic resonance imaging (MRI) is the preferred way to visualize the soft tissue disc and detect internal derangement when indicated. Because TMJ disorders often overlap with muscle-based pain, the care team may collaborate with physical therapists, pain specialists or ENT providers to complete the evaluation.
Most patients respond well to conservative, reversible treatments focused on reducing pain and restoring normal function. Self-care strategies such as eating softer foods temporarily, avoiding hard or chewy items, and limiting wide yawns can reduce strain on the joint. Applying cold for acute swelling or moist heat for tight muscles, along with short-term use of over-the-counter anti-inflammatory medications when appropriate, often provides meaningful relief. Behavioral approaches that reduce clenching, like stress management and habit awareness, are important adjuncts.
Physical therapy and guided jaw exercises help improve mobility, correct muscle imbalances and teach safe movement patterns. Targeted injections may be considered for persistent inflammation or muscle spasm after conservative measures have been tried. When symptoms do not respond, clinicians may discuss occlusal or prosthetic options and, rarely, surgical referral, always prioritizing the least invasive, evidence-based steps first.
Oral appliances such as custom night guards or stabilization splints are commonly prescribed to reduce the effects of bruxism and protect teeth from wear. These devices are made from impressions of the patient’s mouth so they fit comfortably and distribute forces more evenly across the bite. For many patients, a properly fitted appliance reduces muscle activity, decreases joint loading and improves sleep-related grinding.
It is important to understand that oral appliances are a management tool rather than a guaranteed cure for all TMJ disorders. Their effectiveness improves when combined with other therapies such as physical therapy, behavior modification and stress reduction. Regular follow-up is needed to adjust the device as symptoms change and to ensure long-term comfort and protection.
The TMJ and the muscles that control it are closely connected to structures in the head and neck, so dysfunction often manifests as headaches, ear symptoms and neck tension. Referred pain can present as temple or forehead headaches, a sense of ear fullness, tinnitus or soreness behind the ear even when no ear infection is present. Muscle tension from clenching frequently radiates into the neck and shoulders, creating a pattern of multi-site discomfort.
Addressing the jaw mechanics with conservative TMJ therapies often reduces these associated symptoms without needing separate treatments for each complaint. When ear or headache symptoms persist, collaboration with ENT physicians or headache specialists helps rule out non-dental causes and optimize a coordinated treatment plan. A multidisciplinary approach ensures that both joint mechanics and related pain generators are treated effectively.
You should seek specialized care when jaw pain is persistent, worsening or when you experience progressive difficulty opening your mouth, frequent locking, or pain that disrupts sleep and daily activities. Acute trauma to the jaw or sudden changes in bite after dental treatment also warrant prompt evaluation. Early assessment allows clinicians to identify reversible contributors and begin conservative care before chronic changes occur.
During an evaluation our office will perform a focused history and hands-on exam, and arrange imaging or referrals only when necessary to clarify the diagnosis. Working with physical therapists and medical specialists as needed helps create individualized care plans that address both structure and function. Timely intervention typically improves outcomes and reduces the need for invasive procedures.
Changes in how the teeth meet can alter forces across the TMJ and either contribute to symptoms or, in some cases, relieve them if bite relationships are improved. Orthodontic treatment, restorations and prosthetic work must be planned carefully to avoid introducing new imbalances that stress the joint. Occlusal adjustments and definitive dental corrections are considered only after conservative treatments and a thorough evaluation confirm that bite relationships are a significant contributor.
Because the relationship between occlusion and TMJ pain is complex, coordinated planning between the general dentist, restorative specialists and orthodontists produces the best results. Any irreversible dental changes are made cautiously and typically as part of a comprehensive treatment strategy that prioritizes function and patient comfort. Effective communication and stepwise care reduce the risk of unintended consequences and improve long-term outcomes.
You can reduce the risk of developing TMJ problems by limiting activities that strain the jaw, such as chewing hard foods, biting nails or habitual gum chewing. Practicing good posture, especially during long periods of phone or computer use, helps minimize neck and jaw tension. Stress-reduction techniques, adequate sleep and using a custom night guard when grinding is present are practical preventive measures.
If you are concerned about persistent jaw pain or related headaches, schedule an evaluation so a personalized plan can be developed to protect function and comfort. Vaccaro Aesthetic and Family Dentistry provides conservative, evidence-informed TMJ assessment and care and will coordinate referrals when specialized input is needed. Early attention to symptoms allows for less invasive treatment and a better chance of restoring normal jaw function.

Ready to book your next dental visit or learn more about our services?
Getting in touch with Vaccaro Aesthetic and Family Dentistry is quick and easy. Our friendly team is here to help with scheduling, answering questions about treatments, and addressing any concerns. Whether by phone or our convenient online form, we make connecting with us easy. Take the first step toward a healthier, more confident smile—contact us today and experience personalized dental care that truly makes a difference.